 [
[

The brain has its own immune system, which detects threats and mounts a defense. A growing body of evidence has shown that in Alzheimer’s disease, those immune cells are chronically overactivated, causing inflammation that damages the connections between brain cells.
Now, in a preclinical study using human Alzheimer’s brain cells, scientists at Scripps Research have identified a molecular switch—and potential drug target—responsible for driving that chronic inflammation.
The research, published in Cell Chemical Biology on April 23, 2026, centers on a protein called STING, which normally functions as part of the immune system’s early-warning system. In the brains of people with Alzheimer’s, the team discovered that STING undergoes a chemical modification known as S-nitrosylation (or SNO, a reaction involving sulfur, oxygen and nitrogen) that promotes its overactivation. Blocking this chemical change to STING in a mouse model of the disease decreased neuroinflammation.
“This is a new and important therapeutic target for Alzheimer’s disease,” says senior author Stuart Lipton, the Step Family Foundation Endowed Chair at Scripps Research and a clinical neurologist. “It’s exciting to see that blocking this switch in mice reduces inflammation and protects the very brain cell connections that are lost in Alzheimer’s, especially because we found the same pathway to be activated in human Alzheimer’s brain samples and in human stem cell-derived models.”
Over three decades ago, Lipton, who’s also the founding co-director of the Neurodegeneration New Medicines Center at Scripps Research, discovered the S-nitrosylation process, in which a molecule related to nitric oxide (NO) binds to a cysteine amino acid in proteins, producing “SNO” and thus regulates the protein’s function. His lab has shown that SNO—which can be triggered by aging, neuroinflammation and environmental toxins such as air pollution and wildfire smoke—disrupts a variety of different proteins in the body. The modification, causing a veritable “SNO-STORM” to disrupt protein function, has been linked to several human conditions, including cancer, Parkinson’s disease and Alzheimer’s.
In this new study, the team focused on the protein STING, which was previously linked to Alzheimer’s inflammation. Lipton’s group, led by postdoctoral researcher Lauren Carnevale, collaborated with Professor John Yates III, a leading mass spectrometry expert at Scripps Research and holder of the John Lytton Young Endowed Chair. They pinpointed exactly where on STING an S-nitrosylation reaction occurred, homing in on one specific building block of the protein: cysteine 148. When cysteine 148 is S-nitrosylated, they discovered, STING clusters into larger complexes and triggers inflammation.
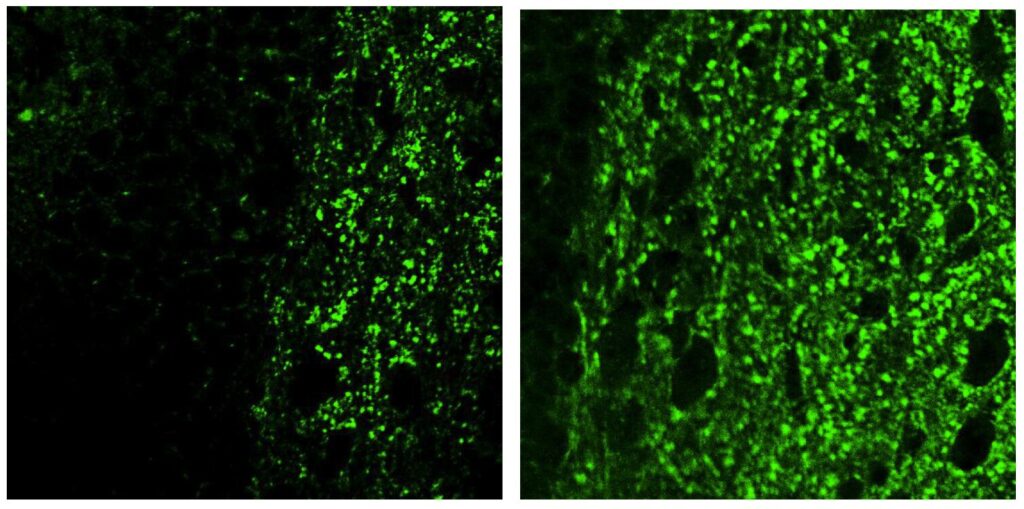
The team found high levels of the chemically modified form of STING (called SNO-STING) in postmortem brain tissue from Alzheimer’s patients, in human brain immune cells grown in the lab and exposed to Alzheimer’s proteins, and in a mouse model of the disease.
In laboratory experiments, the team showed that the clumps of proteins found in the brain in Alzheimer’s—including amyloid-beta and alpha-synuclein—can themselves trigger the S-nitrosylation reaction in STING. This finding suggests that inflammation occurs in a cycle: initial protein clumps, coupled with environmental influences and aging, could cause inflammation that generates NO, driving S-nitrosylation of STING, which in turn drives more inflammation.
The researchers then engineered a version of STING lacking cysteine 148 so it couldn’t be S-nitrosylated. When this modified protein was introduced into a mouse model of Alzheimer’s, brain immune cells showed significantly less inflammation, and critically, the connections between nerve cells (called synapses) were protected from degradation. This preservation of synapses is known to correlate with protection from the cognitive decline of dementia.
“What makes this target particularly promising is that we can quiet the pathological overactivation of STING without shutting down the normal immune response,” says Lipton. “You still need STING to protect yourself from infections, and when we target cysteine 148, we’re not blocking the entire molecule; we’re just preventing STING from becoming overactivated.”
Lipton’s group is now working to develop small molecules that block cysteine 148 for testing in preclinical models.
Publication details
Lauren N. Carnevale et al, Redox regulation of neuroinflammatory pathways contributes to damage in Alzheimer’s disease brain, Cell Chemical Biology (2026). DOI: 10.1016/j.chembiol.2026.03.017
Journal information:
Cell Chemical Biology
Clinical categories
Citation:
How a chemical reaction triggers brain inflammation in Alzheimer’s disease (2026, April 25)
retrieved 25 April 2026
from https://medicalxpress.com/news/2026-04-chemical-reaction-triggers-brain-inflammation.html
This document is subject to copyright. Apart from any fair dealing for the purpose of private study or research, no
part may be reproduced without the written permission. The content is provided for information purposes only.